- Home
- Free Samples
- Health and Safety Management
- 400418 Needs And Stakeholder Analysis...
400418 Needs and Stakeholder Analysis Assessment Answer

400418 Health Advancement and Health Promotion Autumn 2020
Unit Details
Unit Code: | 400418 |
Unit Name: | Health Advancement and Health Promotion |
Credit Points: | 10 |
Unit Level: | 7 |
2.2 Assessment Summary
The assessment items in this unit are designed to enable you to demonstrate that you have achieved the unit learning outcomes. Completion and submission of all assessment items which have been designated as mandatory or compulsory is essential to receive a passing grade.
2.3 Assessment Details
2.3.1 Report - Needs and stakeholder analysis
Weight: | 35% |
Type of Collaboration: | Individual |
Due: | 9 April 2020 |
Submission: | online, via Turnitin on vUWS |
Format: | Word file |
Length: | 1,500 words |
Curriculum Mode: | Report |
A Needs Assessment is:
’a systematic method of identifying unmet health and healthcare needs of a population and making changes to meet these unmet needs. It involves an epidemiological and qualitative approach to determining priorities which incorporates clinical and cost effectiveness and patients’ perspectives. This approach must balance clinical, ethical, and economic considerations of need-that is, what should be done, what can be done, and what can be afforded.’
(Wright, Williams & Wilkinson, 1998)
Your task is to select a target population group and health issue that is in need of a health promotion interven- tion. The target population can be within or outside Australia. Once you have selected your target population and health issue, submit to your tutor for approval.
You are required to individually conduct a Rapid Needs Assessment of the approved target population and health problem. Your aim is to convince a potential funder that the issue you have identified is of high priority, and demon- strate the magnitude of the problem and the existing gaps (the ’need’).
Your Needs Assessment must include:
- Analysis of health needs of target population:
- Health status
- Demography and geography of population
- Social, environmental, and behavioural health determinants
- Analysis of service needs:
- Geography
- Workforce availability
- Efficiency and effectiveness
- Identification of opportunities, priorities and options
- Recommendation of specific actions based on the analysis of the information
A Needs Assessment involves a range of data-gathering methods, including consultation with stakeholders such as specialists and community members. Although it will not be feasible to conduct interviews for this Needs Assessment, it is a crucial step in the process. Therefore, you are required to also conduct a stakeholder analysis.
A stakeholder analysis is an approach to generate knowledge about individuals and organisations so as to understand their “behaviour, intentions, inter-relations and interests; and for assessing the influence and resources they bring to bear on decision-making or implementation processes.”(Varvasovszky & Brugha, 2000)
Your task is to identify at least three stakeholders that you anticipate you would consult with, and engage for, your needs assessment/recommended actions and detail their characteristics by completing the table below. As an exam- ple, the first row has already been completed.
Stakeholder | Description of involvement in the issue | Interest in the issue | Influence/power | Position | Impact of issue on stakeholder |
National Institute of Alcohol | Coordinates national activities in alcohol research, prevention and treatment | High | Low | Supportive | High |
The stakeholder analysis will need to be included in your needs assessment report.
Assessment criteria
- Student locates and critically analyses relevant literature (including peer-reviewed and grey literature, local, state and national strategic plans, and relevant area reports).
- Student synthesises a range of epidemiological and socio-demographic information of the target population and
setting of interest.
- Student analyses the behavioural, environmental, and social contributory factors for the particular health issue of concern and population.
- Student determines priorities for health promotion action from available evidence using local, state and national
data and information collected
- Student applies principles of health promotion to inform thinking about the issue
- Student recommends specific actions based on the analysis of information
- Student includes a brief but comprehensive stakeholder analysis
- Structure and word count
- Correct grammar, syntax
- Referencing
Answer
Report: Needs and Stakeholder Analysis
Executive Summary
This report aims to analyse the needs assessment of Aboriginal and Torres Strait Islanders young people and the health issues like poor nutritional habits and physical inactivity in Indigenous young people, who are in need of a health promotion intervention. For conducting the needs assessment, the Aboriginal and Torres Strait Islanders young people’s health needs, health status, demography and geography has been determined. Moreover, there has been a stakeholder analysis done in this report for which there are three stakeholders including Indigenous young people, NGOs, and Government Department of Health are selected. Furthermore, there has been an action plan provided along with recommendations on particular actions that are mainly based on the evaluation of the information.
Introduction
In this assessment, Needs Assessment will be conducted that will mainly include analysis of health needs of the Aboriginal and Torres Strait Islanders young people, health status, demography and geography of the population of Indigenous young people. Furthermore, the health determinants like poor nutritional habits and physical inactivity in Indigenous young people will be analysed in the needs assessment. Lastly, there will be recommendation provided for the specific actions based on the information’s analysis.
1) Health issues:
Description of the health issue:
The health issue that is identified in this target population group is respiratory diseases like asthma. Asthma is one of the chronic respiratory diseases. People who have asthma face shortness of breath, chest tightness and coughing due to narrow airways. In Australia, 34% disease related burdens are created due to respiratory diseases. The prevalence of asthma among the Torres islander and aboriginal people is high (18%) than the non-indigenous Australians. The rate of asthma is higher among female (20%) than male (15%) (Aihw, 2019). It is seen from the second fact that among young Australians (15 to 24), the rate of asthma is high.
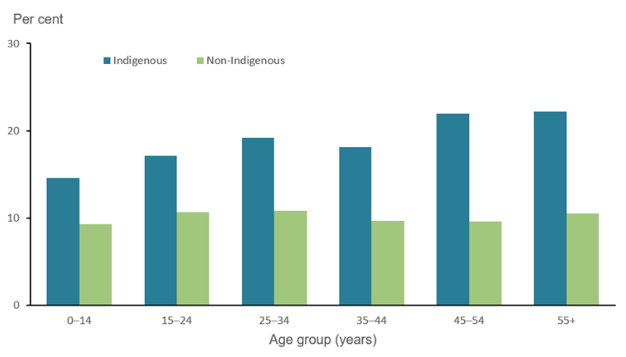
Figure 1: Prevalence of asthma among indigenous and non-indigenous Australian
(Source: Aihw, 2019)
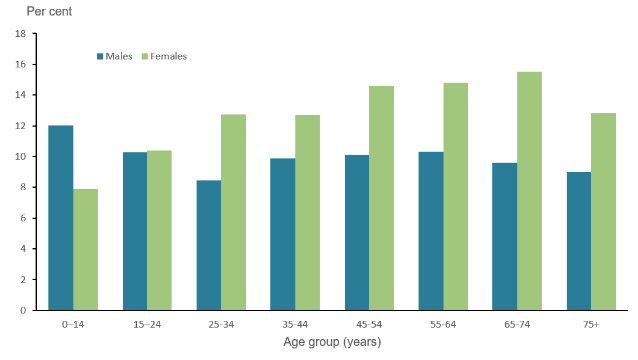
Figure 2: Prevalence of asthma in different age group
(Source: Aihw, 2019)
Overall factors that influence the issue:
The factor that contributes to the development of asthma indigenous Australians are poor access to the specialist’s health care and smoking. Indigenous Australians smokes in higher rate that causes asthma among them. Postnatal and intrauterine exposure to the environmental tobacco smoke creates serious implication on the lung health among young children (Mja, 2019). Hospitalisation rate is high among the indigenous Australian because they are less likely to use inhaled medication for asthma. Indigenous people face more complication in the management of asthma. This is because, there are higher levels of chances to create cardiovascular diseases, comorbid heart related diseases and diabetes among the indigenous Australians (Mja, 2019). Moreover, indigenous people are more likely to deal poor quality of life that creates a serious impact ion the health of indigenous with asthma. Indigenous people who live in non-remote locality are more likely to develop asthma (Mja, 2019). Additionally, pollutants, dietary deficiencies, stress and depressions also created asthma among young aboriginal people.
2) Targeted Population and the impact of health issue
Describe the target population:
The target population group selected in this assessment is Aboriginal and Torres Strait Islanders young people.
According to the statistics available on Australian government website of Australian Institute of Health and Welfare (2018), in every 10 indigenous youth, 6 of them believed that they have a good health (Australian Institute of Health and Welfare, 2018). The analyses of disease’s burden demonstrate that for the Indigenous young people, who are aged between 10–24 years, the main contributors to the particular disease burden has been road traffic accidents (6 percent), alcohol use disorders (7 percent), anxiety disorders (8 percent) and self-inflicted injuries and suicide (13 percent) (Australian Institute of Health and Welfare, 2018). Moreover, a decline is noticed in the mortality rate of the young Indigenous individuals in years from 2005 to 2015; 70 per 100,000 to 67 per 100,000 (Australian Institute of Health and Welfare, 2018). Besides, the recorded deaths in years 2011–2015 for the Indigenous individuals aged between 10–24 years is 674. Poisoning and injury led to most of the deaths, including assaults, land transport accidents and suicides (Australian Institute of Health and Welfare, 2018).
Description of the health issue in target population:
There has been a big difference between life expectancy for Aboriginal people and non-Aboriginal people aged 17 and over. Aboriginal and Torres Strait Islander young people have poor health compared to other non-Australians (Azzopardi, et al., 2018). The Indigenous young people mortality rate for those under 65 is more than twice the Indigenous young people (Penrose, et al., 2018). Indigenous young people do not have access to equal health care opportunities as other Australian communities and populations. Compared to other Australian populations, indigenous peoples experience the disadvantages of socio-economic exposure, when exposed to dangerous environments and behavioural health factors. It has been observed that the rate of asthma is very common among indigenous people. However, the rate of asthma is higher among people among 35 years and more. However, there are higher levels of chances that young indigenous people are also affected by asthma.
Factors influencing the issue on target population:
The key health determinants in indigenous young people that will be discussed in this assessment include poor nutritional habits and physical inactivity. Improving the health of indigenous peoples has long been recognized by the Australian Government as a continuing problem (Phillips & Luke, 2017). Differences in health status between Australia’s non-aboriginal and aboriginal population have long been unacceptable. When indigenous young people continue practicing the unhealthy lifestyles due to lack of knowledge, it leads them to fall in the category of obese people (Blake, et al. 2019).
Further, due to illiteracy, the unhealthy eating habits of these young people are associated to various chronic and acute health problems like diabetes, heart disease, stroke and hypertension along with increased mortality rates (Krusz, et al., 2019; Belton et al., 2018).
Impact on target population:
The treatment process of asthma requires huge costs. Therefore, in some cases, it is highly difficult for the indigenous people in bearing the costs of treatment which increases the rate of death.
Having asthma among indigenous people create affect on schooling, employment, personal relationship, social interaction and emotional wellbeing (Brożek et al. 2017). After having asthma people always experience some impact on their life.
Asthma also creates higher level of impact on asthma. Physical impact of asthma ranges from occasional cough to the life threatening condition (Bousquet et al. 2018). The seriousness as well as frequency of asthma is always dependent on the overall severity of asthma and how it can be controlled (Brożek et al. 2017). Complications that can be created among people include permanent narrowing bronchial tubes, the side effects of medication and risks of obesity. For some people, asthma can create chronic inflammation of the airways which can lead to the structural change in airways. Structural change in the airway can be created a loss in the lung function, chronic coughing, developed mucous glands, wall thickening of airways (Bousquet et al. 2018).
Asthma can increases depression and anxiety among people which can cause panic attack among people. Depression and anxiety may limit the ability of self-management of asthma.
3) Service capabilities and community resources:
Resource exists in the community to address the health issue:
For offering a better care to the indigenous people in treating asthma, it is important in involving large number of health workforce. After involving the health workforce, it is necessary in distributing the health workforce based on the requirements (Chung et al. 2018). For example, huge number of workforce must be distributed in those locations where the number of affected people is high. On the other hand, the less number of workforces must be allocated in those location where the number of affected people is less. After that, it is necessary in spreading the health services in remote areas so that it can help the indigenous people in getting an effective asthma related care (Everard et al. 2015). For offering an effective asthma care, it must be regularly monitored and controlled so that its efficiencies can be managed. Along with that, the healthcare facilities must be affordable to the indigenous people so that they can access healthcare and get an effective physical and mental well-being.
Stakeholder analysis:
Refer to appendix 1.
4) Action Plan
The plan is to increase access for Indigenous young people by reducing barriers and barriers to access. This can be achieved by increasing the geographical distribution of healthcare in remote areas. Other ways are needed to ensure that all Indigenous young people have access to primary and preventive health care, as people cannot travel from their home suburbs where health care is important (Bailie, et al., 2017). This mainly involves establishing well-resourced medical facilities in rural areas and providing medical assistance and sufficient staff. Besides, Aboriginal and Indigenous individuals should seek unequal government support and increase employment in all sectors (Loutfi, et al., 2018).
This needs to be done in several ways, including the application process, career development, mentoring and available meetings, and the cultural awareness and education and training needs of the Aboriginal and Indigenous residents. Besides, there are occurrence and occurrence gaps between Aboriginal communities and non-Aboriginal people.
Recommendations
The recommendation includes:
- The remote government should develop policies to strengthen the even distribution of care in remote areas. This will reduce the number of hospitalized patients due to preventable diseases in indigenous communities, reducing inequalities in quality of life and health.
- Governments, NGOs, local authorities and health professionals should come together to provide community camp activities and advise them on key social health factors that interfere with people’s health.
Conclusion
In conclusion, it could be stated that the barriers to better health care are important because Aboriginal people and towers have lower health and life expectancy than Aboriginal people. This is due to the preventive and primary care, insufficient educational opportunities, lack of government support, unemployment, housing estates’ remote and unequal distribution within the society, and other health’s social determinants. Further research on the same literature is needed to develop existing policies and literature that could be utilised for protecting the future generations’ health.










